Consequences of Sepsis
Whilst the consequences are often dependent on the bacterium or virus responsible, they are usually dramatic and severe. So time is of the essence.
Sepsis may not necessarily result from the infection. To help with a prompt diagnosis, your clinicians should be trying to exclude the possibility of sepsis - rather than assuming it isn’t present.
The ‘quick SOFA’ score (sequential organ failure assessment) is used where sepsis should be diagnosed if a patient has any 2 of these symptoms:
- Increased breathing rate
- A change in their level of consciousness
- Low blood pressure.
Medical imaging also helps to identify the possible source of the infection.
What Happens after Diagnosis?
Once a sepsis diagnosis has been made, 6 steps should be taken within the next hour:
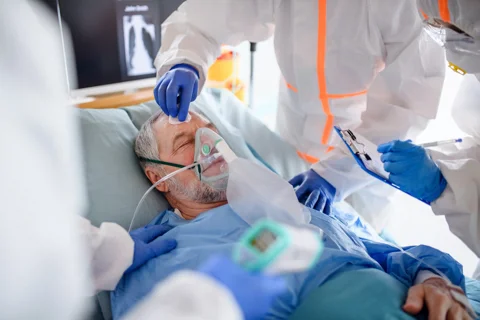
- Improve oxygen levels
- Take blood samples
- Administer intravenous antibiotics
- Measure the build-up of lactate levels
- Rebalance fluid levels
- Accurately measure urine output.
These steps are called the ‘Sepsis Six’ and are the current international standard. They aim to ‘identify’, ‘treat’ and ‘prevent deterioration’.
Treatment will often occur in Intensive Care and a properly experienced specialist will need to carefully assess the nature and extent of your injury. The amount and type of treatment will likely require careful consideration by the medical team and different doctors may have different views.
The medical staff must still act within an acceptable range of medical opinion in providing the treatment and in attempting to prevent other injuries arising. Even if the treatment successfully kills the initial infection and stops the sepsis, patients may suffer severe consequences.
For example, the long-term organ damage, cognitive impairment, breathing difficulties and reduced mobility can all occur in extreme cases.
And unfortunately, sepsis can be fatal.
Can I Claim Compensation?
As with any medical condition, it’s important not to jump to the wrong conclusion. But while doctors are highly trained and cases of negligence are rare, sometimes things do go wrong, and you should be prepared for this.
In those circumstances, it may be appropriate to seek compensation after trying the official NHS Complaints Procedure.
Contact us for a free consultation and we’ll be happy to help you.